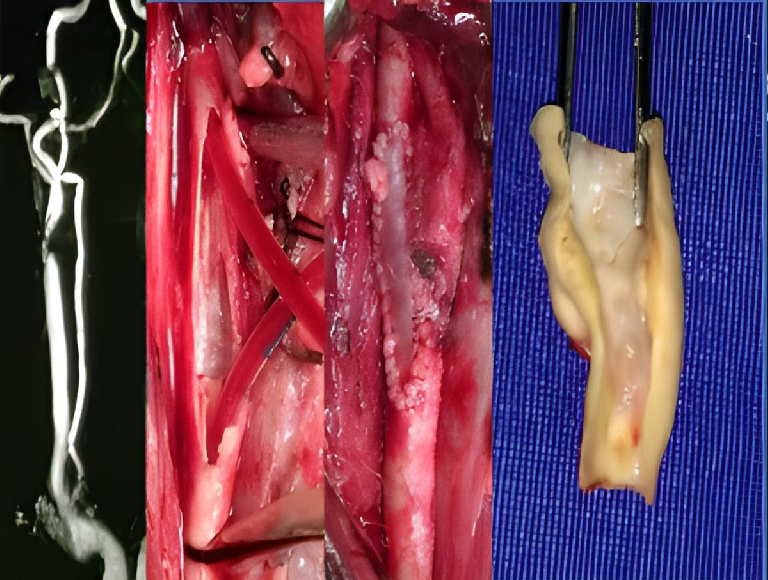
This is an open surgical procedure where the carotid artery is exposed and the plaque is physically removed from within the artery. The artery is then closed with the help of a vein or graft patch to make the vessel wider and prevent future narrowing. This technique is called patch plasty.
CEA is performed under general or local anesthesia and usually takes around 2 hours. It is one of the most effective and time-tested methods for preventing stroke in patients with severe carotid artery disease.
Benefits of Carotid Endarterectomy
- Direct removal of the plaque
- Lower chance of emboli (clots) going to the brain
- Durable results with long-term patency
- Highly effective in both symptomatic and asymptomatic high-grade stenosis
This procedure is generally recommended for patients with more than 70 percent blockage or those who have suffered a TIA or minor stroke.
In patients who are at high surgical risk or when anatomy favors a minimally invasive approach carotid artery stenting (CAS) is performed. This procedure is done through a small puncture in the groin and guided under X-ray.
A thin tube called a catheter is advanced into the carotid artery. Before crossing the plaque a filter device called an embolic protection device is placed beyond the blockage. This filter captures any debris that might dislodge during the procedure. Then a stent is deployed to hold the artery open and restore smooth blood flow.
Advantages of Carotid Stenting
- Minimally invasive
- No surgical incision in the neck
- Shorter hospital stay
- Faster recovery
- Ideal for elderly and high-risk patients
The procedure is done under local anesthesia and patients are usually discharged within a day or two.
These are office-based procedures done under local anesthesia or sedation. The goal is to seal the faulty veins from inside, so blood flows through healthier veins.
Endovenous Laser Ablation (EVLA)
- A thin fiber is inserted into the vein, and laser energy is used to seal it shut.
- No cuts, stitches, or hospitalization required.
- Quick recovery, minimal pain.
Radiofrequency Ablation (RFA)
- Uses heat via radio waves to close off the vein.
- Similar outcomes to laser, with low complication rates.
Endovenous Glue Therapy
- A special medical glue is used to seal the vein.
- No thermal energy or post-op stockings needed.
- Ideal for needle-phobic or elderly patients.
Microwave Ablation
- A newer modality that uses microwave energy.
- Efficient in treating large-caliber veins with minimal heat spread.
Sclerotherapy
- Suitable for smaller veins and cosmetic concerns (spider veins).
- A medicine is injected into the vein, causing it to collapse and fade.
- Performed alongside endovenous procedures.
- Tiny incisions are made to hook out bulging veins.
- Helps reduce symptoms and improves cosmetic appearance.
- Removal of the entire saphenous vein via open surgery.
- Rarely done today due to the success of endovenous techniques.
- Reserved only for select cases where endovenous access isn’t possible.