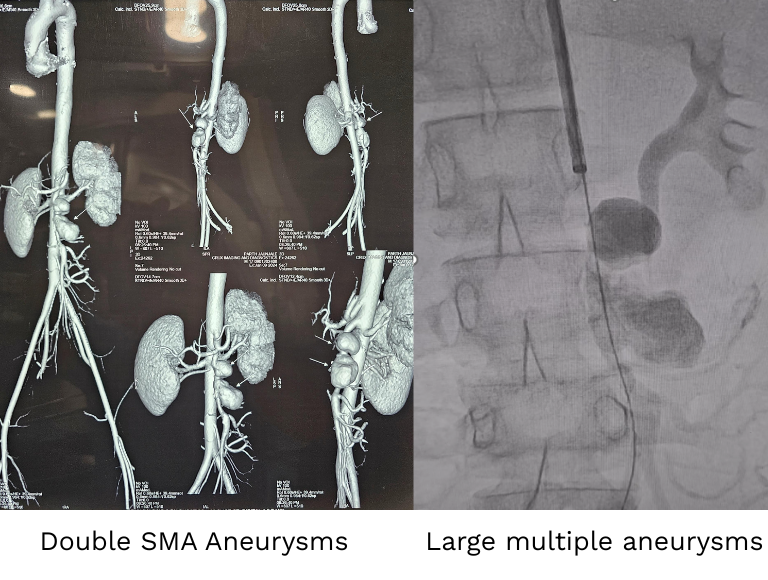
Once the bleeding artery is identified during angiography, embolisation is performed to block the blood flow. This is done by injecting special materials like coils, glue, or particles into the artery.
Benefits:
- No large incision required
- Precise control of the bleeding vessel
- Less pain and faster recovery
- Can be done even in critically ill patients
Embolisation is effective in most cases of arterial GI bleeding or mesenteric bleeds. It can be repeated if needed.
In cases where embolisation is not possible or if there is additional bowel injury, open surgery is required. The bleeding vessel is tied off or repaired. If part of the bowel has died due to lack of blood supply, that segment may need to be removed.
Indications for surgery:
- Patient unstable despite embolisation
- Presence of perforation or bowel gangrene
- Large aneurysm or pseudoaneurysm requiring repair
- Failed non-surgical attempts
Surgical intervention is life-saving in these situations and is performed by a vascular surgeon with experience in abdominal vessels.