In AVMs where blood flow is rapid the feeding arteries are blocked using agents like coils, glue or alcohol. This reduces the pressure in the malformation and makes it more manageable. The procedure is done through a small puncture in the groin or arm and is guided by imaging.
Benefits of embolisation:
- Minimally invasive
- Reduces size and bleeding
- May be used as a standalone treatment or before surgery
Multiple sessions may be needed especially in large or complex AVMs. Complete cure may not be possible with embolisation alone if the nidus remains active.
In slow flow malformations like venous or lymphatic types a sclerosant is injected directly into the lesion. This causes the vessel walls to scar and shrink. The treatment is usually done under ultrasound guidance and may require multiple sittings.
Sclerotherapy is useful for:
- Venous malformations in limbs or face
- Lymphatic cysts or swellings
- Lesions that are not accessible by surgery
Mild swelling or pain may occur after the procedure but it usually settles in a few days.
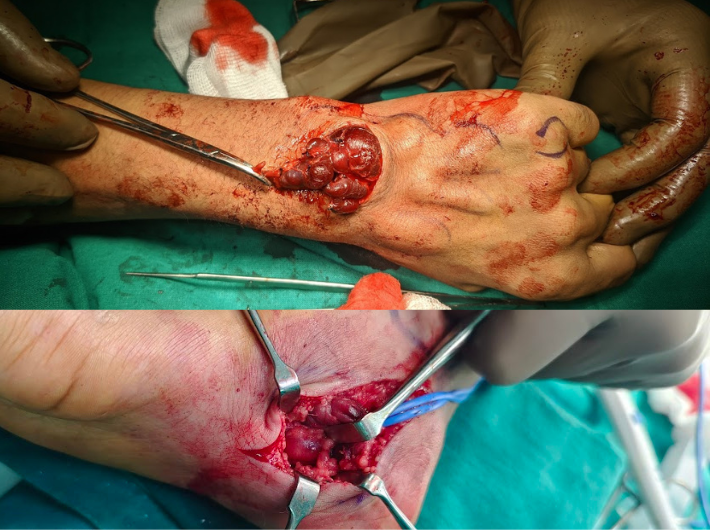
When the malformation is localised and accessible surgical removal may be advised. This is especially important in large AVMs where the nidus is clearly defined and can be completely removed. Excision is also considered when embolisation or sclerotherapy is not enough to control symptoms.
Points to remember:
- Surgery may follow embolisation to reduce bleeding risk
- Cosmetic outcome is better when complete excision is achieved
- Partial removal may lead to recurrence or worsening
Surgery is done under anaesthesia and requires expert planning to avoid damage to nearby structures.
Extensive swelling with skin hardening, deformity, nodules or ulcers. Limb becomes very heavy and functionally limited.
- Removal of the entire saphenous vein via open surgery.
- Rarely done today due to the success of endovenous techniques.
- Reserved only for select cases where endovenous access isn’t possible.